Iowa Model of Evidence-Based Practice
1. Introduction
Importance of Evidence-Based Practice in Healthcare
- Evidence-based practice (EBP) is essential for improving patient care, safety, and healthcare outcomes.
- Modern healthcare systems rely on evidence-based nursing and nursing research to guide clinical decisions rather than tradition or routine practice.
- Frameworks such as the Iowa Model of evidence-based practice help healthcare professionals translate research findings into clinical practice that consistently supports quality care, particularly in complex environments such as critical care.
Brief Introduction of the Iowa Model of Evidence-Based Practice
- The Iowa Model of evidence-based practice is a widely recognized framework developed at the University of Iowa to guide the implementation of evidence-based practice in healthcare organizations.
- Often called the Iowa Model, this structured approach helps nurses and clinicians identify problems, review nursing research, and implement practice change strategies that improve patient care and outcomes.
- Through ongoing revisions and validation, the Iowa Model of evidence-based practice continues to evolve, ensuring that healthcare teams effectively integrate evidence-based practice to promote safer and more effective treatment.
Purpose and Scope of the Article
- This article explores how the Iowa Model of evidence-based practice supports the translation of nursing research into real-world clinical practice.
- Readers will learn how the Iowa Model provides a systematic process for identifying practice problems, evaluating research evidence, and implementing sustainable practice change initiatives.
- The discussion will also highlight how the Iowa Model of evidence-based Practice encourages collaboration through the Iowa Model Collaborative, enabling healthcare teams to apply evidence-based practice to promote improved patient care.
- Ultimately, the framework helps organizations revise current procedures and strengthen practice to promote quality care.
Why the Iowa Model Is Influential and Practical
- The Iowa Model of evidence-based practice is influential because it provides a clear, step-by-step framework for integrating evidence-based nursing into daily clinical practice.
- Developed at the University of Iowa, the Iowa Model emphasizes teamwork, structured decision-making, and systematic evaluation to guide the implementation of evidence-based practice across healthcare settings.
- Its focus on identifying clinical triggers, evaluating nursing research, and applying evidence ensures meaningful practice change that improves patient care outcomes.
- With ongoing revisions and validation led by the Iowa Model Collaborative, the Iowa Model of evidence-based practice remains a practical and reliable framework that helps nurses consistently deliver quality care, particularly in specialized settings such as critical care, while strengthening practice to promote quality care.
2. Background and Origins
History: Development of the Iowa Model and Its Creators
- The Iowa Model of evidence-based practice was developed in the early 1990s at the University of Iowa Hospitals and Clinics to guide nurses in integrating evidence-based practice into daily clinical practice.
- Nurse researchers and leaders at the University of Iowa recognized the need for a structured framework to translate nursing research findings into real-world patient care improvements.
- The Iowa Model of evidence-based practice, often referred to as the Iowa Model, was designed to help clinicians identify practice problems, review research evidence, and implement practice change strategies effectively.
- Over time, the model gained national recognition as a practical approach to the implementation of evidence-based practice across healthcare settings, including critical care environments.
The Context of Evidence-Based Practice When the Model Emerged
- When the Iowa Model of evidence-based practice emerged, healthcare organizations were increasingly recognizing the importance of evidence-based nursing to improve patient care outcomes.
- Many nurses relied heavily on tradition and experience, while nursing research findings were often underutilized in clinical practice.
- The Iowa Model was introduced during a period when healthcare systems sought systematic approaches to integrate evidence-based practice to promote better outcomes and reduce variations in care.
- By providing a clear process for identifying triggers for practice change, the Iowa Model of evidence-based practice helped healthcare teams translate evidence into practice to promote quality care, especially in high-risk settings such as critical care.
Foundational Principles and Goals of the Model
- The Iowa Model of evidence-based practice is grounded in the belief that healthcare decisions should be guided by the best available nursing research, clinical expertise, and patient preferences.
- A central goal of the Iowa Model is to support the implementation of evidence-based practice that directly improves patient care and outcomes.
- The model encourages healthcare teams to evaluate clinical problems, review research evidence, and develop structured strategies for practice change within clinical practice environments.
- Collaboration is a key component of the Iowa Model of evidence-based practice, particularly through initiatives such as the Iowa Model Collaborative, which supports shared learning and dissemination of evidence-based practice to promote safer care.
- Continuous revisions and validation ensure that the Iowa Model of evidence-based practice remains relevant as healthcare knowledge evolves.
- Organizations using the Iowa Model are encouraged to revise outdated protocols and strengthen practice to promote quality care, ensuring that evidence-based nursing becomes a routine part of healthcare delivery.
3. Core Components and Structure of the Iowa Model
Overview: Flowchart and Decision Points
- The Iowa Model of evidence-based practice is structured as a clear flowchart that guides nurses through the implementation of evidence-based practice in healthcare settings.
- Developed at the University of Iowa, the Iowa Model of evidence-based practice uses decision points that help clinicians determine whether sufficient nursing research exists to support practice change.
- The Iowa Model helps healthcare professionals integrate evidence-based nursing into clinical practice while ensuring that decisions improve patient care and strengthen practice to promote quality care across healthcare environments, including critical care units.
Triggering Issues: Problem-Focused vs. Knowledge-Focused Triggers
- A central feature of the Iowa Model of evidence-based practice is the identification of triggers that initiate the implementation of evidence-based practice.
- Triggers represent issues that signal the need for improvement in clinical practice or patient care outcomes.
- Two major trigger types within the Iowa Model of Evidence-Based Practice include:
Problem-focused triggers
- Arise when issues such as increased infection rates, medication errors, or inconsistent patient care outcomes are identified.
- These problems prompt healthcare teams to review nursing research and consider practice change strategies that enhance quality care.
- For example, a critical care unit experiencing increased ventilator-associated pneumonia may use the Iowa Model to guide evidence-based interventions.
Knowledge-focused triggers
- Occur when new nursing research, guidelines, or innovations suggest improved approaches to clinical practice.
- The Iowa Model of evidence-based practice encourages healthcare teams to assess whether emerging evidence supports evidence-based practice to promote better patient care.
- By identifying these triggers, the Iowa Model of evidence-based practice ensures that healthcare organizations systematically evaluate opportunities for improvement.
Forming a Team and Assembling Resources
- The Iowa Model of evidence-based practice emphasizes the importance of interdisciplinary collaboration in the implementation of evidence-based practice.
- Once a trigger is identified, healthcare organizations form a team of clinicians, nurse leaders, educators, and researchers to guide the project.
- This team reviews relevant nursing research, clinical guidelines, and institutional resources to support effective practice change.
- Collaborative initiatives such as the Iowa Model Collaborative further support healthcare teams by sharing best practices and tools that strengthen evidence-based nursing and improve patient care outcomes.
Critically Appraising Evidence and Synthesizing Findings
- In the Iowa Model of evidence-based practice, teams carefully evaluate available nursing research to determine the strength and reliability of the evidence.
- Critical appraisal ensures that healthcare professionals rely on high-quality studies when planning practice change within clinical practice.
- The Iowa Model encourages clinicians to compare research findings, identify patterns, and synthesize results to guide the implementation of evidence-based practice.
- Through this process, healthcare teams ensure that evidence-based practice to promote improved patient care is supported by credible data.
- Continuous revisions and validation of the Iowa Model of evidence-based practice reinforce its effectiveness in guiding evidence-based nursing initiatives across healthcare systems.
Piloting Practice Change and Evaluating Outcomes
- Before implementing changes widely, the Iowa Model of evidence-based practice recommends piloting the proposed practice change in a controlled clinical setting.
- Pilot testing allows healthcare teams to observe how new interventions affect patient care and determine whether adjustments are needed.
- For example, a critical care team may introduce a new infection prevention protocol based on nursing research and monitor its impact on patient outcomes.
- Data collected during the pilot phase helps clinicians evaluate whether the implementation of evidence-based practice leads to measurable improvements in quality care.
- If necessary, teams may revise strategies before expanding the initiative across the organization.
Implementing and Disseminating Successful Changes
- When pilot testing confirms positive outcomes, the Iowa Model of evidence-based practice supports the full implementation of evidence-based practice across healthcare units.
- Healthcare organizations integrate successful interventions into policies, protocols, and routine clinical practice to ensure consistent patient care improvements.
- The Iowa Model also encourages sharing results through professional education, publications, and collaborative networks such as the Iowa Model Collaborative.
- Disseminating findings helps healthcare organizations revise outdated practices and strengthen practices to promote quality care, ensuring that evidence-based nursing continues to advance healthcare outcomes.
4. Step-by-Step Application: Practical Example
Scenario Selection: Common Clinical Problem
- A common scenario used to demonstrate the Iowa Model of evidence-based practice is the reduction of catheter-associated urinary tract infections (CAUTIs) in hospitalized patients.
- Healthcare organizations frequently identify CAUTIs as a preventable safety issue that affects patient care outcomes and increases healthcare costs.
- Using the Iowa Model of evidence-based practice, nurses can evaluate clinical practice procedures related to catheter insertion and maintenance.
- This approach supports evidence-based nursing and helps healthcare teams apply evidence-based practice to promote safer interventions and improve quality care.
- The Iowa Model encourages systematic practice change based on nursing research, particularly in high-risk environments such as critical care units.
Identifying the Trigger and Forming the Team
- In the Iowa Model of evidence-based practice, the first step is identifying a triggering issue that signals the need for improvement in patient care.
- A hospital may observe an increase in catheter-associated infections, making it a problem-focused trigger for practice change.
- Using the Iowa Model of evidence-based practice, nurse leaders form a multidisciplinary team that may include bedside nurses, infection control specialists, nurse educators, and physicians.
- The Iowa Model emphasizes collaboration to support the implementation of evidence-based practice within clinical practice settings.
- Many healthcare systems also collaborate with initiatives such as the Iowa Model Collaborative, which shares resources developed by the University of Iowa to strengthen evidence-based nursing and improve practice to promote quality care.
Searching and Appraising Evidence: Methods and Key Sources
- The Iowa Model of evidence-based practice requires healthcare teams to conduct a systematic search for nursing research related to the clinical problem.
- Databases such as PubMed, CINAHL, Cochrane Library, and professional nursing journals provide reliable sources of evidence supporting evidence-based practice.
- Using the Iowa Model, the team reviews guidelines, randomized trials, and quality improvement studies addressing catheter care protocols.
- Researchers assess study quality, relevance, and applicability to clinical practice to ensure safe patient care improvements.
- The Iowa Model of evidence-based practice encourages critical appraisal and synthesis of findings to identify best practices that support evidence-based practice to promote infection prevention.
- Through revisions and validation, healthcare organizations ensure that recommendations derived from nursing research align with current clinical standards and can support effective practice change.
Developing and Piloting an Intervention Based on Evidence
- After reviewing the evidence, the Iowa Model of Evidence-Based Practice guides healthcare teams in developing an intervention based on the best available research.
- For example, the team may implement a catheter care bundle that includes sterile insertion techniques, daily catheter necessity assessments, and improved documentation procedures.
- The Iowa Model recommends piloting the intervention within a selected unit, such as a critical care department, before expanding it across the organization.
- This step ensures that the implementation of evidence-based practice is feasible within real clinical practice settings.
- Nurses evaluate whether the intervention improves patient care outcomes and supports practice to promote quality care.
- The Iowa Model of evidence-based practice ensures that interventions are tested carefully before widespread practice change occurs.
Measuring Outcomes, Revising, and Scaling Up
- In the final stage of the Iowa Model of evidence-based practice, healthcare teams measure outcomes to determine whether the intervention successfully improves patient care.
- Key indicators may include reduced infection rates, improved documentation compliance, and enhanced adherence to evidence-based nursing protocols.
- Data analysis helps clinicians evaluate whether the implementation of evidence-based practice achieved the intended goals.
- If necessary, teams may revise the intervention based on outcome data and feedback from clinicians working in clinical practice.
- Continuous revisions and validation ensure that improvements remain effective over time.
- Once successful, the Iowa Model of evidence-based practice supports scaling the intervention across departments and sharing results through networks such as the Iowa Model Collaborative.
- This process ensures that healthcare organizations consistently apply evidence-based practice to promote safer care and sustain practice change that improves quality care.
5. Strengths and Benefits
Facilitates Systematic Decision-Making and Collaboration
- The Iowa Model of evidence-based practice provides a structured framework that supports systematic decision-making in evidence based practice within healthcare organizations.
- Developed and widely applied at the University of Iowa Hospitals and Iowa Hospitals and Clinics, the model helps nurses translate research evidence into practical improvements in nursing care delivery.
- Using the Iowa Model, healthcare teams within the Department of Nursing Services collaborate to guide nursing care decisions and implement evidence-based interventions at the point of care.
- The steps of the Iowa Model encourage interdisciplinary teamwork and strengthen research and evidence based practice, helping clinicians integrate research evidence in nursing practice.
- As a result, evidence-based practice implementation becomes more organized and effective, supporting the delivery of quality care and strengthening practice among nurses across healthcare settings.
Supports Contextual Adaptation and Clinician Engagement
- The Iowa Model of evidence-based practice, also referred to as the Iowa Model of EBP, encourages clinicians to adapt research and evidence to their local healthcare context.
- Healthcare professionals using the Iowa Model frameworks can tailor clinical practice guideline recommendations to fit specific patient populations and healthcare settings, such as the intensive care unit.
- This adaptability supports the use of evidence-based practice in nursing practice at a tertiary hospital and other healthcare environments where practice among nurses varies.
- The Iowa Model revised structure also helps address perceived barriers to evidence-based practice and improves clinician engagement in evidence-based practice in nursing.
- Through collaboration with organizations such as the College of Nursing and the Office of Nursing Research in Iowa City, the Iowa Model of Evidence-Based Practice continues to promote evidence-based practice competencies for practicing registered nurses and advanced practice nurses.
Promotes Measurable Improvements in Patient Outcomes
- A key strength of the Iowa Model of evidence-based practice is its ability to translate research into practice through systematic evaluation of evidence-based interventions.
- The application of evidence-based strategies helps healthcare organizations improve the quality of care and enhance the delivery of evidence-based nursing care.
- EBP using the Iowa Model allows clinicians to evaluate the delivery of care to patients and measure outcomes such as infection rates, patient safety indicators, and improved nursing care practice.
- By strengthening evidence-based practice among nurses, the model helps healthcare teams improve nursing care and promote excellence in healthcare.
- Continuous evaluation ensures that interventions following the Iowa Model produce meaningful improvements in care to patients, particularly in complex clinical settings.
Examples of Documented Successes in Practice
- The Iowa Model of evidence-based practice has been successfully used in nursing to implement evidence-based practice in the prevention of hospital-acquired infections and improve nursing care delivery.
- Healthcare organizations using the Iowa Model have reported improved output utilization in clinical practice, stronger attitudes and practices regarding evidence-based practice, and enhanced delivery of care to patients with fever and other acute conditions.
- These successes demonstrate how evidence-based nursing care guided by the revised model helps healthcare systems promote excellence in health care and sustain improvements in clinical practice.
6. Limitations and Criticisms
Resource and Time Constraints for Frontline Staff
- Although the Iowa Model of evidence-based practice is widely used in nursing, frontline staff may face challenges when using the Iowa Model due to limited time and staffing.
- Nurses working in busy settings such as the intensive care unit often prioritize immediate care to patients, leaving little time for research into practice activities.
- Even in advanced institutions like the University of Iowa Hospitals and Clinics, implementing evidence-based practice across nursing services and patient care units can require significant resources.
- Staff within the Department of Nursing Services must balance clinical duties with reviewing research evidence in nursing practice, which can create perceived barriers to evidence-based practice and slow the delivery of quality care.
Challenges in Evidence Availability or Quality
- Another limitation of the Iowa Model of evidence-based practice involves gaps in high-quality research evidence needed to support evidence-based intervention decisions.
- In some clinical areas, particularly emerging fields of practice in nursing, sufficient research and evidence-based practice data may not exist.
- When EBP using the Iowa Model is attempted without strong clinical practice guideline support, healthcare teams may struggle to translate research evidence in nursing practice into effective nursing care delivery.
Potential Barriers to Sustainability and Scaling
- Sustaining improvements achieved through the Iowa Model of evidence-based practice can be challenging in large healthcare systems.
- Organizations must maintain evidence-based practice competencies for practicing registered nurses and advanced practice nurses to support the delivery of evidence-based nursing care.
- Without ongoing education from institutions such as the College of Nursing and the Office of Nursing Research in Iowa City, the Iowa Model revised framework may face barriers to scaling interventions following the Iowa Model and maintaining consistent quality of care.
7. Comparison with Other EBP Models
Comparison with Other Evidence-Based Practice Models
- The Iowa Model of evidence-based practice is one of several widely recognized evidence-based practice models used in practice in nursing to translate research evidence into clinical improvements.
- Compared with the Johns Hopkins Nursing Evidence-Based Practice Model, which emphasizes the PET process, the Iowa Model of Evidence-Based Practice focuses on identifying triggers and applying the steps of the Iowa Model to guide evidence-based practice implementation.
- The PARIHS framework emphasizes context and facilitation, whereas using the Iowa Model emphasizes structured decision points for research into practice and evidence-based intervention at the point of care.
- Healthcare organizations such as the University of Iowa Hospitals and Clinics have demonstrated how evidence-based practice in nursing strengthens nursing care delivery and improves quality of care.
- These evidence-based practice models help address perceived barriers to evidence-based practice and strengthen practice among nurses.
Unique Features of the Iowa Model and When It Is Preferable
- The Iowa Model of evidence-based practice stands out because it integrates research evidence in nursing practice with structured teamwork across nursing services and patient care units.
- Using the Iowa Model frameworks within the Department of Nursing Services supports EBP using the Iowa Model to guide nursing care decisions and implement interventions following the Iowa Model.
- Institutions such as the College of Nursing and the Office of Nursing Research in Iowa City contributed to the Iowa Model revised framework, which continues to promote excellence in health care and improve nursing care across settings such as the intensive care unit.
8. Recommendations for Implementation
Strategies for Leadership Support and Resource Allocation
- Successful adoption of the Iowa Model of evidence-based practice requires strong leadership commitment and organizational support.
- Healthcare leaders should allocate resources that support evidence-based practice to promote excellence in clinical practice.
- Hospitals and academic centers can strengthen evidence-based nursing by embedding the Iowa Model of evidence-based practice within practice at an academic medical institution and aligning it with a model of strategic quality improvement initiatives.
- Addressing clinical practice and perceived barriers, and understanding practice and perceived barriers among clinicians, improves the state of evidence-based practice and helps healthcare teams implement interventions in nursing more effectively.
Building EBP Capacity: Training, Mentors, and EBP Champions
- The Iowa Model of evidence-based practice supports the establishment of evidence-based practice competencies through ongoing education and mentorship.
- Training programs should integrate education and clinical care experiences that strengthen evidence-based practice in US nurses.
- Mentorship from advanced practice nurses in real-world clinical environments helps guide staff nurses in translating research into practice-based nursing and midwifery practice.
Practical Tips for Sustaining Improvements and Measuring Impact
- Healthcare organizations using the Iowa Model of evidence-based practice should regularly evaluate outcomes to ensure improvements are sustained.
- Monitoring patient outcomes and clinician engagement helps confirm that evidence-based practice across medical specialties is improving care delivery.
- Continuous evaluation ensures the Iowa Model of evidence-based practice remains effective after teams have validated the model through practice outcomes.
9. Future Directions and Research Opportunities
Areas for Refinement of the Model and Integration with Digital Tools
- The Iowa Model of evidence-based practice continues to evolve as healthcare systems integrate digital health technologies and decision-support tools.
- Future refinements of the Iowa Model of evidence-based practice may include integrating electronic health records and data analytics to strengthen evidence-based practice and promote excellence in clinical practice.
- Digital platforms can support evidence based nursing by improving access to research and reducing clinical practice and perceived barriers among clinicians.
- These innovations can enhance the state of evidence-based practice and strengthen practice at an academic medical center and other healthcare institutions.
Opportunities for Research: Implementation Science and Outcome Studies
- The Iowa Model of evidence-based practice presents opportunities for research within implementation science and outcome evaluation.
- Researchers can examine how intervention in nursing guided by the Iowa Model of evidence-based practice influences patient outcomes and the establishment of evidence-based practice competencies among clinicians.
- Studies focusing on evidence-based practice in US nurses and practice nurses in real-world clinical settings can further validate the model.
Encouraging Interdisciplinary Adoption Beyond Nursing
- The Iowa Model of evidence-based practice can expand beyond evidence-based nursing to support evidence-based practice across medical disciplines.
- Interdisciplinary collaboration involving advanced practice nurses in real-world clinical settings and other healthcare professionals strengthens education and clinical care experiences.
- This approach promotes evidence-based nursing and midwifery practice and encourages broader application of the model in healthcare systems.
Boost Your Nursing Grades
Struggling with a nursing assignment? Ivy Nursing Help provides expert writers, evidence-based research, and APA-perfect papers to help you submit confidently and score higher.
10. Conclusion
Recap of Key Points and the Value of the Iowa Model
- The Iowa Model of evidence-based practice provides a structured framework that helps healthcare professionals translate research into practical improvements in patient care.
- By supporting evidence-based nursing and encouraging intervention in nursing, the Iowa Model of evidence-based practice strengthens decision-making in modern healthcare.
- The framework helps address clinical practice and perceived barriers and improves practice and perceived barriers among clinicians implementing change.
- Through systematic processes, the Iowa Model of evidence-based practice has validated the model as an effective approach for implementing evidence-based practice to promote excellence in healthcare delivery.
Final Thoughts on Advancing Evidence-Based Practice in Healthcare
- Moving forward, the Iowa Model of evidence-based practice will continue to play a critical role in improving the state of evidence-based practice and strengthening evidence-based practice in US nurses.
- Healthcare institutions should prioritize the establishment of evidence-based practice competencies and integrate education and clinical care experiences that prepare advanced practice nurses in real-world clinical environments.
- Expanding evidence-based practice across medical disciplines, including based nursing and midwifery practice, will further strengthen patient outcomes.
- Ultimately, the Iowa Model of evidence-based practice supports a model of strategic improvement that advances high-quality healthcare worldwide.
11. FAQs: Iowa Model of Evidence-Based Practice
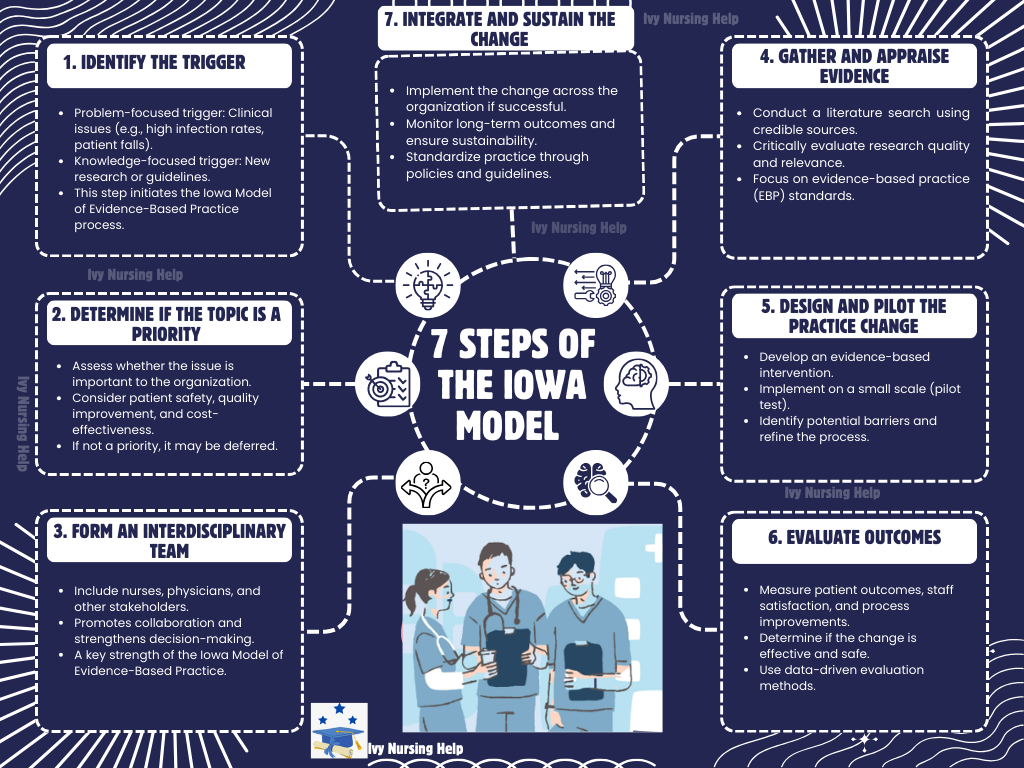
What are the 7 steps of the Iowa model?
- The Iowa Model of evidence-based practice provides a structured process to guide evidence-based practice in clinical practice.
- The Iowa Model typically includes identifying triggers, determining priorities for practice change, forming a team, gathering nursing research, evaluating evidence, piloting interventions, and implementing successful improvements.
- Developed at the University of Iowa, the Iowa Model of evidence-based practice helps nurses apply evidence-based nursing to improve patient care and strengthen practice to promote quality care, especially in complex environments like critical care.
What are the 5 phases of the Stetler model?
- The Stetler model is another framework supporting the implementation of evidence-based practice in healthcare.
- Its five phases include preparation, validation of nursing research, comparative evaluation, decision-making, and application of findings in clinical practice.
- Like the Iowa Model of evidence-based practice, the Stetler model helps translate evidence-based practice to promote excellence and supports practice change based on strong research evidence.
How many steps are there in the Iowa model?
- The Iowa Model of evidence-based practice is commonly described as having seven key steps that guide the implementation of evidence-based practice.
- These steps focus on identifying clinical issues, reviewing nursing research, testing interventions, and integrating successful changes into clinical practice.
- Through revisions and validation, the Iowa Model of evidence-based practice continues to evolve to support quality care and improve the state of evidence-based practice.
What are the models of evidence-based practice?
- Several frameworks guide evidence-based practice in healthcare, including the Iowa Model of evidence-based practice, the Johns Hopkins model, the Stetler model, and the PARIHS framework.
- These models support evidence-based nursing and encourage healthcare teams to translate nursing research into patient care improvements.
- The Iowa Model of evidence-based practice, supported by initiatives such as the Iowa Model Collaborative, is widely used to guide evidence-based practice in US nurses and strengthen practice at an academic medical institution.
